EDITOR'S NOTE: This article is part of an ongoing SooToday series — 'Turning the Tide' — that explores potential solutions to our city’s toxic drug crisis. You can read more about our project HERE.
Eight years after eight people were poisoned by toxic drugs in a single night, community leaders and front-line workers are reflecting on how that moment marked a turning point for Sault Ste. Marie’s ongoing battle with opioids.
In 2017, local community partners assembled to respond to the increase in drug poisonings, referred to at the time as overdoses.
By definition, an overdose is the body's response to too high a dose of a substance, but what was happening on the streets and behind closed doors in the Sault was something different.
The local drug supply was being poisoned with dangerous and sometimes fatal amounts of cyclopropyl fentanyl.
Desiree Beck was employed as an outreach worker with the Hep Care Program at the Group Health Centre and was asked to chair the Sault Ste. Marie and Area Drug Strategy.
"In 2016, we really started to see the massive spike in overdoses, but to be very clear, no one wanted to hear about it. Nobody," Beck said.
She spent much of her time at the now-shuttered Neighbourhood Resource Centre on Gore Street, which opened in 2014 but closed during the pandemic.
"I volunteered a lot there and we did a lot of drug education, I mean like right down to the cops," Beck said. "We showed people how to use their crack pipes properly with police officers there — it was a weird time."
That partnership was on full display on Nov. 2, 2017 when Beck and Sonny Spina, who at the time was a member of the Sault Police Service, worked together to write a press release after local emergency services responded to the eight people who were poisoned by drugs overnight.
The release offered information on what to look for in a drug poisoning and the benefits of naloxone, a medication that reverses the effects of opioids.
Spina recalled that difficult day and, almost eight years later, said he has some regrets about how that was worded.
"When looking back now, I read this article and I cringe at my own words, because I used the words overdose instead of opioid poisoning. But that's what we knew at the time, I guess," he said.
Earlier that year, in April, Spina moderated a town hall public information session that was held at The Machine Shop.

Beck was one of the keynote speakers who addressed the crowd about the opioid crisis and the need for more naloxone kits to be available to people who use drugs.
"That one particular meeting certainly highlighted the fact that this was in every corner of our community and it also was able to highlight how many service providers are out there," said Spina.
When the Sault Police news release came out regarding the eight drug poisonings in one night, Algoma Public Health was already ramping up its opioid response with community partners.
APH began receiving funding in 2017 for harm reduction initiatives, including naloxone distribution and training, opioid overdose surveillance and coordination with partners for local opioid response.
From the time the province's Office of the Chief Coroner began releasing its statistical data on opioid deaths, overdoses and hospitalizations in May of 2017, it was clear Sault Ste. Marie was more adversely affected than almost anywhere else in Ontario.
Launched with 10 years worth of data, the OCC's online opioid tracking tool showed Algoma ranked second among 36 Ontario public health unit locations when it explored opioid-related emergency room visits and hospitalizations.
The numbers have fluctuated since then.
In 2018, there were 26 confirmed and probable opioid-toxicity deaths reported in Sault Ste. Marie.
That number went down to 16 in the following year, only to climb to 34 in 2020 — the first year of the pandemic.
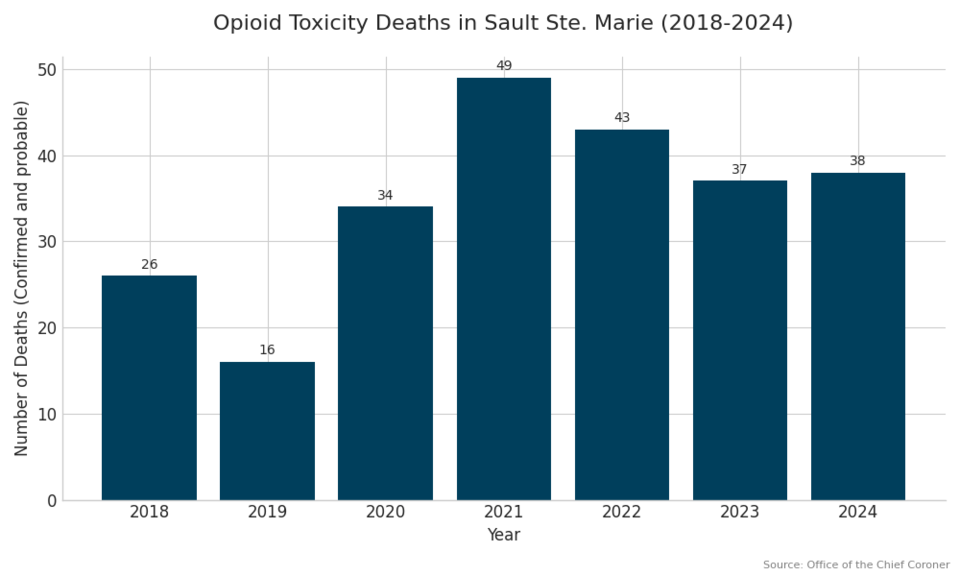
Once the pandemic hit, the opioid crisis in the city was brought into full public view, a phenomenon that continues to this day.
Spina stepped down from the police in 2021 to enter the private sector and political life. As a Conservative candidate in the 2021 federal election, Spina criticized the Liberal government's handling of the opioid crisis.
Beck went on to launch Willow Addiction Services with the intention of setting up a supervised consumption site in the Sault.
She said the organization is now defunct after the provincial Progressive Conservative government closed the door for such sites in Ontario.
Between 2018 and 2024, a total of 243 people in Sault Ste. Marie died from opioid toxicity, or poisoned drugs, according to the OCC.
Beck moved to Sault Ste. Marie in 2009 to work at the Group Health Centre at a time when Algoma Public Health's needle exchange program was operated only two hours per week.
"I started operating a needle exchange out of my office whenever people needed it and the city was really against that," said Beck.
As the evidence of drug use became more visible, she said some of the blame from the public came back to the work she was doing.
"It went from being a hidden issue to a very public issue and a lot of people attributed that to the increase in needle-syringe programs or access to sterile supplies, but we know that's bullshit.
“The reason that it was actually turning more public is because in the background of all these things we had, the secondary issues like the housing crisis were boiling underneath.
“We saw buildings being condemned and more and more people were displaced," Beck said.
Connie Raynor-Elliott, founder of Save Our Young Adults from Drug Addiction, has been helping people living with addiction at the street level for almost 15 years.
She believes the true number of people lost to poisoned drugs may be much higher.
Raynor-Elliot began looking into the Sault's drug culture around 2010, when OxyContin was the drug of choice for many.
"When my son admitted that he was addicted to Oxy, I started researching it, calling helplines, and I brought him to our detox," said Raynor-Elliott.
That's when she hit her first major roadblock with the system and reached out to others through Facebook for support.
"They were basically saying they didn't have any room. He needs to go to detox, but there's no room and it's like what do you do?" said Raynor-Elliott.
"So that's when I literally sat in front of the laptop and said, 'Is anybody else out there?'"

SOYA was founded in 2011 after the shocking death of one of her son's 18-year-old friends from a fatal drug poisoning.
"I actually started SOYA because we were watching the kids die and nobody was doing anything," said Raynor-Elliott.
Raynor-Elliott said despite the best efforts of many in the community, the stigma against people who live with addiction continues.
"People have to remember, that is somebody's kid — I don't care how old they are, that's somebody's kid.
“A lot of our community is very generous — if you need something, they're there — you'll see people that hand out water and you know they want to help.
“But I'd like to see a lot more. I'm going to be honest. I see a lot more help than before. We've come a long way, but we have a long way to go.”
Paramedic Chief Katie Kirkham was a commander with the Sault Ste. Marie Paramedic Services in 2017. She recalls how surprised and unsettled members of the service were by the sudden rise in overdoses around the time those eight poisonings happened.
"What struck me most was how these incidents marked a shift in our community — overdoses went from being unusual, almost rare, to something our paramedics are exposed to far more often. Sadly, what once felt exceptional has now become commonplace," she said.
Kirkham said that also reshaped how the community needed to respond, with greater collaboration, stronger supports and wider access to harm reduction strategies like naloxone.
"It’s also made it clear that we need to rethink and refine our strategies for the future, to continue offering the best care for the community," said Kirkham.




